Trapped by Your ZIP Code: How 10 States Created Healthcare Deserts for the Poor
6.1 min read
Updated: Dec 20, 2025 - 13:12:43
Whether a low-income family faces medical bankruptcy or a $75 copay often depends on which side of a state line they live. Ten U.S. states continue to reject Medicaid expansion under the Affordable Care Act, leaving about 1.6 million adults in a “coverage gap”, earning too much to qualify for Medicaid but too little for federal subsidies. This policy choice has measurable costs in lives lost, billions in forfeited federal funding, and worsening health inequalities. For families in non-expansion states like Texas and Alabama, the gap translates directly into unaffordable medical bills and preventable deaths.
- Coverage gap: Nearly 1.9 million Americans in 10 non-expansion states earn above strict Medicaid cutoffs (e.g., 18% of federal poverty level) but below subsidy thresholds.
- Financial fallout: Texas forfeited $9.2B in federal funds in 2022, while families face $40k–$50k hospital bills without coverage.
- Health impact: Medicaid expansion linked to 12 fewer deaths per 100,000 adults annually; 15,600 preventable deaths occurred in non-expansion states.
- Equity gap: 65% of people in the coverage gap are people of color; most are working but uninsured in low-benefit industries.
- Policy stakes: Expansion would increase state Medicaid spending by just 3%, offset by savings on uncompensated care.
The state you call home can determine whether a medical issue is a minor inconvenience or a financial disaster. For low-income Americans, living in one of the 10 states that refused Medicaid expansion means a single hospital visit could trigger financial catastrophe that might take decades to recover from, if ever.
A family of four in Texas earning $6,200 annually faces a $47,000 emergency appendectomy bill with no insurance coverage. Three hundred miles away in Louisiana, which expanded Medicaid, the same family earning $5,400 annually would pay a $75 hospital copay for identical surgery.
The difference between financial ruin and financial security lies in an arbitrary line drawn by state governments when they chose whether to expand Medicaid under the Affordable Care Act.
This decision has created what health policy experts call the “coverage gap”, more than 1.6 million adults between ages 19 and 64 are trapped in this coverage gap across all non-expansion states, earning too much to qualify for Medicaid but too little to receive federal subsidies for private insurance.
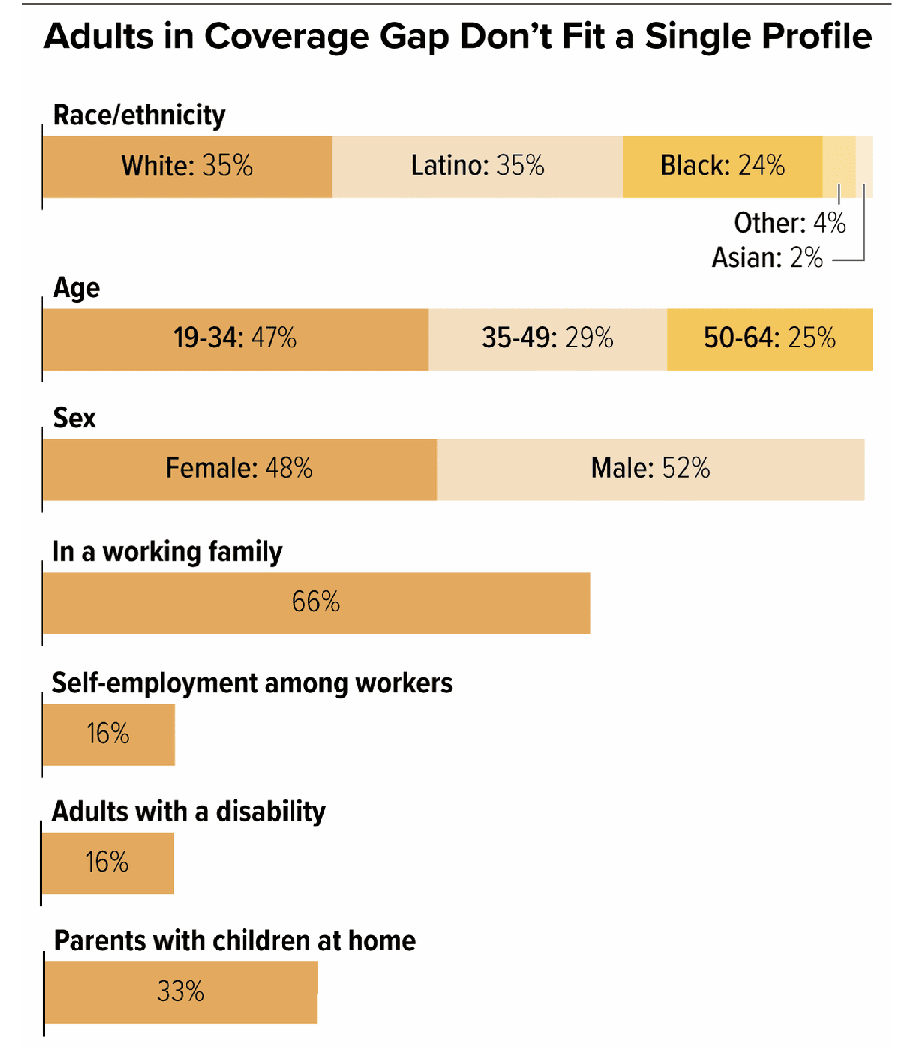
Source: CBPP
Understanding Poverty Level Percentages
The federal poverty level is the government’s official measure of what constitutes poverty in America. In 2024, the poverty line for a family of three is set at $25,820 per year. When states use percentages like “18% of the federal poverty level,” they’re setting income limits far below even this basic poverty threshold.
For example, 18% of the poverty level for a family of three equals just $4,678 annually, that’s roughly $390 per month or $90 per week for an entire family. To qualify for Medicaid in Texas, your family would have to be making less than that.
To put this in perspective, that’s less than many people spend on groceries alone. These extremely low thresholds mean that families can be desperately poor- earning just a few thousand dollars per year – yet still ‘make too much’ to qualify for Medicaid in non-expansion states.
The Mathematics of the Coverage Gap
An estimated 1.9 million Americans in those 10 states are within the Medicaid coverage gap. The income thresholds reveal the severity:
- Texas: Adults without children are ineligible for Medicaid regardless of income; parents must earn less than 18% of federal poverty level ($4,678 annually for a family of three)
- Alabama: 18% of federal poverty level for parents
- Expansion states: Up to 138% of federal poverty level ($20,780 for an individual in 2024)
In Alabama and Mississippi, more than a quarter of uninsured working-age adults are left with no affordable pathways to health coverage. Texas has the largest population of people in the cohort, accounting for 41% of people in the coverage gap.
Financial Impact of Non-Expansion
Ten states have refused federal funding to expand Medicaid: Alabama, Florida, Georgia, Kansas, Mississippi, South Carolina, Tennessee, Texas, Wisconsin, and Wyoming.
The financial impact is substantial:
- Texas: Forfeited $9.2 billion in federal funds in 2022 alone
- Florida: Lost $5 billion in federal funding
- Georgia: Lost $2.9 billion
Federal funding would cover approximately 93% of the cost of insuring new populations, with states responsible for only 7%. Taxpayers in states not participating in the Medicaid expansion bear a share of the overall cost, without benefitting from the program.
Health Outcomes: The Life and Death Data
Research consistently demonstrates that Medicaid expansion saves lives:
- According to NBER research, the ACA’s expansion of Medicaid saved the lives of at least 19,200 adults aged 55 to 64 over four years from 2014 to 2017
- At the same time, 15,600 older adults died prematurely because of state decisions not to expand Medicaid
- Among 32 expansion states and 17 non-expansion states, Medicaid expansion was associated with nearly 12 fewer deaths per 100,000 adults annually
An estimated 39 to 64 percent reduction in annual mortality rates for older adults gaining coverage. Mortality changes were closely linked to county-level coverage gains, with one life saved annually for every 239 to 316 adults gaining insurance.
In Texas alone, with 617,000 people in the coverage gap, this translates to an estimated 1,950 to 2,582 preventable deaths annually.
Border State Disparities
State boundaries create dramatic healthcare inequalities. A University of Michigan study found that Illinois averted 345 deaths annually while Missouri had 194 additional deaths each year. The same trends held for Kentucky (expansion) versus Tennessee (non-expansion), and New Mexico (expansion) versus Texas (non-expansion).
Dr. Karen Joynt Maddox at Washington University noted that when treating Medicaid patients from Illinois, doctors know procedures and medicines will likely be covered. With uninsured Missourians, they must consider whether patients can afford follow-up medications after heart attacks.
Limited Solutions
For those in the coverage gap, conventional solutions don’t work:
Residency Requirements: Medicaid requires genuine legal residency with documentation. Temporary relocation for medical benefits constitutes fraud.
Emergency Care Limitations: Federal law requires emergency stabilization but doesn’t cover chronic disease management, prescriptions, or preventive care.
Community Health Centers: Provide sliding-scale care but have limited capacity and often lack specialist services.
The Coverage Gap Population
People in the coverage gap are racially and ethnically diverse, and 65% are people of color. Childless adults account for 76% of the coverage gap. Most people in the coverage gap have jobs but work in industries less likely to provide health insurance coverage, such as service industry or construction.
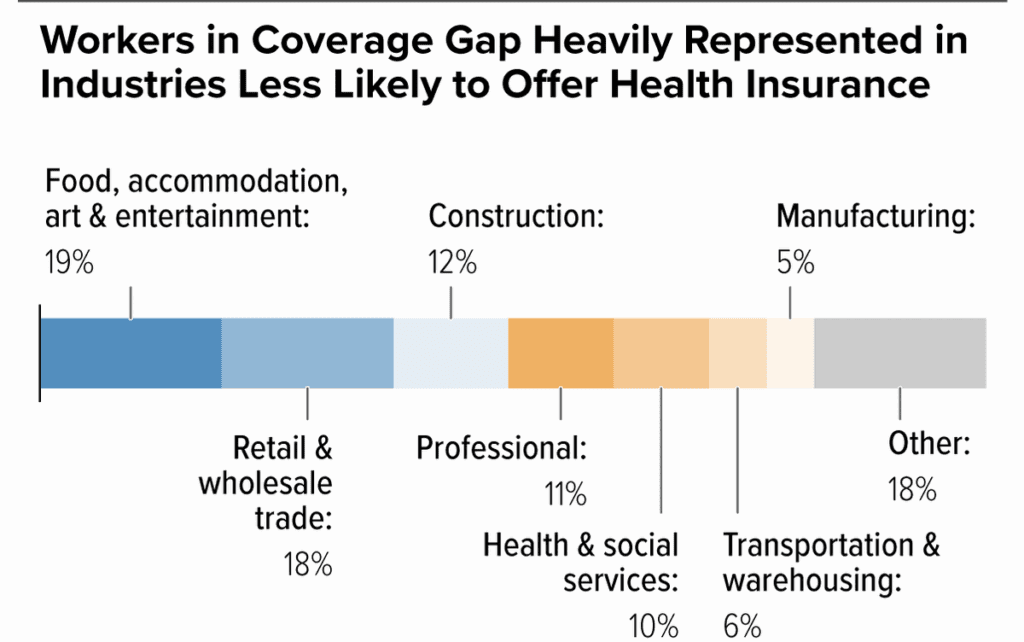
Source: CBPP
The median income limit for eligibility in the traditional Medicaid program is 38% of the FPL in non-expansion states. The uninsured rate within non-expansion states was 15.4% in March 2023 compared to 8.1% in expansion states.
Economic Pressures for Change
Recent Urban Institute estimates show that if the ten remaining non-expansion states implemented Medicaid expansion in 2024, their Medicaid spending would increase by only 3% or $1.5 billion, partially offset by $457 million in state and local government savings on uncompensated care.
GOP power brokers in Mississippi, Alabama and Georgia suggest there might be an opening to expand eventually, citing economic competition concerns. Georgia Republican Sen. Chuck Hufstetler noted: “We need healthy workers” as the state competes for industrial investments.
Conclusion
The data is unambiguous: Medicaid expansion saves lives, saves money, and improves health outcomes. Ten states still have not adopted the ACA’s Medicaid eligibility expansion, leaving 1.5 million of some of the poorest people in the country uninsured.
The coverage gap represents a quantifiable policy failure measured in preventable deaths, foregone federal funding, and deteriorating health outcomes. Until these states act on available evidence, 1.6 million Americans remain trapped by geography, their health outcomes determined by arbitrary state boundary lines rather than medical need or empirical data.