Inside the Claims Process: How Insurers Actually Approve or Deny Your Claim
12.3 min read
Updated: Dec 28, 2025 - 23:12:11
Insurance claims follow a structured, contract-driven process, not a discretionary one. Insurers evaluate every claim against policy language, medical-necessity standards, and procedural requirements, not personal circumstances. Most denials stem from administrative errors, unmet prior authorization rules, or coverage limits rather than permanent exclusions. Understanding how claims are screened, reviewed, and adjudicated, and knowing your appeal rights, can materially improve your chances of payment and help you correct denials that are often reversible.
- Administrative review comes first: Insurers initially verify coverage status, filing deadlines, and documentation; many early denials are due to correctable errors like coding mismatches or missing information.
- Prior authorization is a major gatekeeper: Failure to obtain required pre-approval is one of the most common denial reasons, even when services are otherwise covered.
- Medical necessity drives payment decisions: Approval depends on whether services meet evidence-based guidelines and your policy’s definition of necessity, regardless of physician preference.
- Many denials are overturned on appeal: More than half of appealed private-insurer denials are ultimately paid, often after fixing documentation or coding issues.
- You have formal appeal rights: ACA-compliant plans must offer internal and independent external reviews with strict timelines and written explanations tied to policy language.
When you file an insurance claim, you are entering a structured process governed by your policy contract, applicable regulations, and the insurer’s claims procedures. Many policyholders only encounter this process after a loss, which can create confusion when expectations about coverage, timing, or payment do not align with how claims are actually evaluated.
Most claim disputes arise from misunderstandings about policy terms, deductibles, exclusions, or documentation requirements. Insurers assess claims strictly against the language of the policy, not on perceived fairness or personal circumstances. Understanding how claims are reviewed, and why they may be delayed, reduced, or denied, can help you navigate the process more effectively and avoid common pitfalls.
The Initial Claim Review
Every claim begins with a first notice of loss. Whether you report an accident to your auto insurer, submit medical bills to your health plan, or notify your homeowners carrier about property damage, this initial contact triggers a standardized review process.
The first assessment is primarily administrative. Does the policy exist and is it active? Was the claim filed within required timeframes? Are all necessary forms and documentation included? Is the claimant covered under the policy?
Administrative errors account for a meaningful share of early claim denials. According to ACA marketplace transparency data, roughly one in five claims submitted to marketplace insurers in 2023 were denied, though denial rates vary significantly by insurer and plan. Common non-substantive reasons include incorrect patient information, billing code errors, or missing documentation, issues that are often resolved through correction and resubmission.
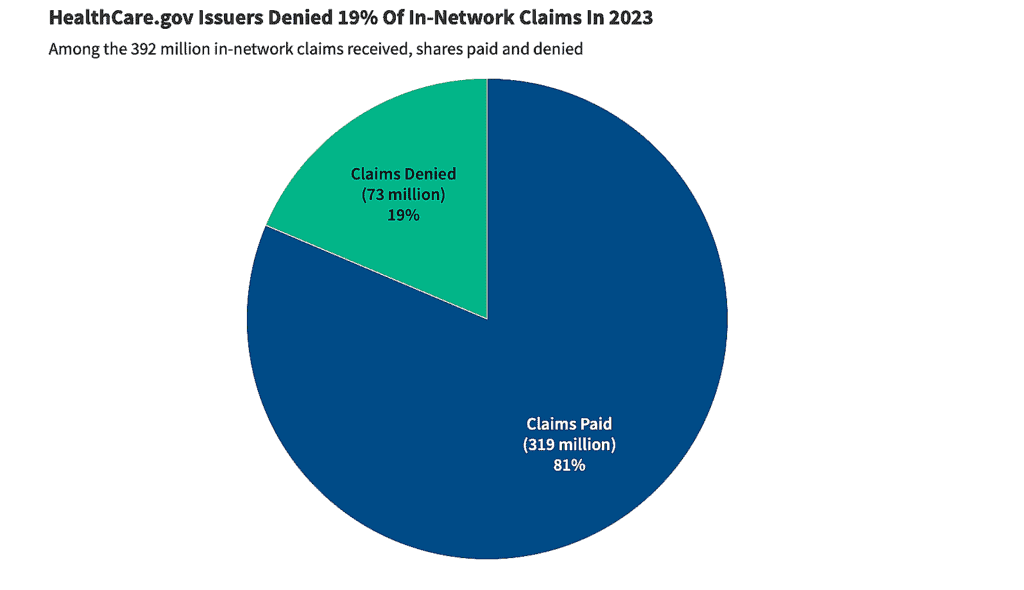
Source: KFF
This administrative review typically happens quickly, often within days. Automated systems flag straightforward problems such as coverage gaps, identification mismatches, or lapsed policies. These checks are procedural in nature and occur before any evaluation of medical necessity, liability, or policy interpretation.
Prior Authorization: The Pre-Approval Gatekeeper
For many health services, prior authorization represents the first real decision point in the claims process. Before you receive certain non-emergency services, the insurer must approve them as medically necessary and covered under your policy terms. Comparable pre-approval requirements can also exist in some property insurance situations, though they are less standardized than in health insurance.
Prior authorization has become a major friction point in the insurance system. Failure to obtain required prior authorization is consistently cited as one of the leading reasons health insurance claims are denied, particularly in provider surveys and insurer transparency reports. The process requires a healthcare provider to submit clinical documentation showing that the proposed treatment meets the insurer’s medical necessity and coverage criteria.
Insurers argue that prior authorization helps prevent unnecessary or low-value care and controls costs. Critics counter that it can delay medically necessary treatment and impose significant administrative burdens on providers and patients. In response, some states have enacted reforms regulating the process. Texas’s “gold card” law, for example, allows physicians with consistently high approval rates for specific services and insurers to bypass prior authorization requirements, though participation remains limited and varies widely by specialty and payer.
The prior authorization decision occurs before treatment is delivered. If authorization is denied, you generally face three options: proceed with the service and pay out of pocket, pursue an alternative covered treatment, or appeal the denial. Emergency care is exempt from prior authorization requirements, although authorization may still apply to non-emergency or post-stabilization services that follow.
Medical Necessity Determination
Even when prior authorization is granted, or for services that do not require it, insurers still assess whether treatment meets the policy’s definition of “medical necessity” when the claim is reviewed. Prior approval does not guarantee payment if the service ultimately falls outside coverage criteria.
Medical necessity reviews are conducted by licensed clinical professionals, such as nurses or physicians employed by or contracted with the insurer or a utilization management vendor. Reviewers evaluate whether the service aligns with generally accepted standards of medical practice for the diagnosed condition, using evidence-based guidelines, clinical literature, and the specific policy language defining covered benefits.
Disputes arise because medical necessity is not always clear-cut. A treating physician may view a treatment as the most appropriate option, while the insurer’s reviewer may determine that it is not sufficiently supported by evidence, is considered experimental, or does not meet the plan’s medical policy requirements. These disagreements typically reflect differing interpretations of medical evidence and policy terms rather than bad faith.
Recent scrutiny has focused on insurers’ use of algorithms and automated tools in utilization review. While such systems are commonly used to support claim triage and consistency, applicable regulations require human clinical judgment in medical necessity determinations. Lawsuits have alleged that certain insurers, including UnitedHealthcare, relied on algorithm-driven tools in ways that contributed to improper denials. These claims remain contested.
Step Therapy and Other Coverage Requirements
Many health insurance plans use step therapy, which requires patients to try lower-cost treatments before approving more expensive alternatives. If a doctor prescribes a brand-name medication, the insurer may require the patient to try a generic or preferred drug first. Coverage for the higher-cost option is typically approved only if the initial treatment is ineffective, not tolerated, or medically inappropriate, as documented by the provider.
Plans may deny coverage if required steps are not followed, but most include formal exception and appeal processes. While step therapy is designed to control costs by directing patients toward treatments that work for many people, it can delay access to specific therapies for individuals who need more immediate or specialized care.
Coding Accuracy and Technical Denials
A significant share of claim denials result from coding or billing errors rather than true coverage disputes. Medical claims rely on standardized procedure codes, such as Current Procedural Terminology (CPT), along with diagnosis codes. If a claim contains an incorrect, outdated, or mismatched code that does not support the billed service, automated systems may deny it.
For example, a service may be coded as preventive when it was diagnostic, or a deprecated procedure code may be used. These technical denials are usually administrative rather than substantive and are often correctable through resubmission with accurate coding. However, they can still cause delays and confusion for patients who receive denial notices for services they reasonably expected to be covered.
The Adjudication Process
Once a claim passes initial screening, it enters adjudication, the formal evaluation of whether the service or loss qualifies for payment under the policy. During this stage, claims professionals, such as adjusters, examiners, or clinical reviewers, depending on the type of insurance, apply policy language to the specific facts of the claim.
The reviewer examines all relevant documentation, which may include medical records, provider notes, diagnostic reports, photos of property damage, police reports, or other supporting evidence based on the claim type. These details are compared against policy provisions, exclusions, limitations, and coverage criteria.
Insurers may request additional information during adjudication. In health insurance, this typically involves reviewing complete medical records to assess medical necessity and consistency with evidence-based guidelines and policy requirements. In property insurance, the insurer may send a staff adjuster, independent adjuster, or third-party inspector to evaluate damage in person. Failure to provide requested documentation can result in denial.
The length and complexity of adjudication vary widely. A straightforward auto claim with clear liability and standard repairs may be resolved within days, while more complex claims, such as workers’ compensation cases involving permanent disability, can require months of investigation, independent medical examinations, and legal review.
Why Claims Get Denied
Understanding common denial reasons helps you avoid them or challenge them appropriately when they occur:
- Service not covered under policy terms: The treatment, procedure, or loss isn’t included in your specific policy. This isn’t an error, it reflects the limits of your coverage.
- Exclusions apply: The claim falls under a policy exclusion, such as intentional acts or specifically excluded perils like flood or earthquake. In health insurance, pre-existing condition exclusions apply only to non-ACA plans; ACA-compliant plans cannot deny coverage on that basis.
- Benefit limits reached: You’ve exhausted applicable coverage limits, such as annual visit caps for services like physical therapy or skilled nursing care. Lifetime dollar limits are prohibited for essential health benefits under ACA-compliant plans but may exist in non-ACA or supplemental policies.
- Out-of-network provider: You received care from a provider outside your plan’s network. Depending on policy terms, this may result in no coverage or higher cost-sharing.
- Treatment deemed experimental or investigational: The insurer determines the treatment lacks sufficient evidence or broad clinical acceptance under its coverage criteria, even if your physician believes it’s appropriate.
- Lack of medical necessity: The insurer’s reviewing clinician concludes the service doesn’t meet medical-necessity standards based on clinical guidelines and policy definitions.
- Administrative errors: Incorrect patient information, wrong or mismatched billing and diagnosis codes, missing documentation, or procedural submission errors can trigger denials.
A 2024 hospital survey found that 51.7% of initially denied claims were later overturned and paid, with private insurers overturning 54.3% of denials, indicating that many denials stem from correctable administrative or documentation issues rather than permanent coverage exclusions. However, appealing and correcting denials carries a cost: providers spend an average of $43.84 per appealed claim for private payers, contributing to billions of dollars in administrative expense across the healthcare system.
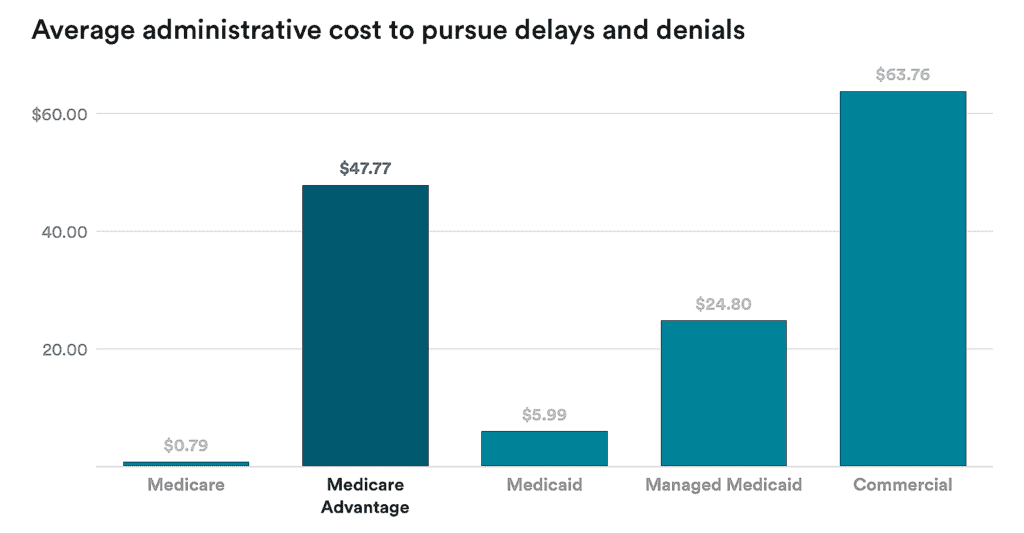
Source: STAT News
The Human Element
Claims decisions are not made solely by automated systems, though automation plays an increasingly large role, particularly in high-volume and routine claims. Depending on the insurance type and claim complexity, decisions may be made through automated rules engines, human review, or a combination of both.
When human reviewers are involved, claims professionals apply their training and internal guidelines to interpret policy language and claim documentation. Experienced adjusters or reviewers can identify legitimate claims that warrant approval, especially in complex or ambiguous cases. However, inconsistency in policy interpretation, rigid internal criteria, or incomplete documentation can result in denials that may later be reversed.
Documentation remains critical. In health insurance and many other regulated insurance contexts, insurers are generally required to provide written explanations for claim denials, citing relevant policy provisions or medical criteria and outlining appeal rights. These explanations provide transparency and give claimants the information necessary to correct errors or pursue an appeal.
Your Appeal Rights
If your claim is denied, you generally have legally protected appeal rights under the Affordable Care Act (ACA) for most ACA-compliant health insurance plans. The ACA established standardized appeal processes with mandatory timelines to ensure claims receive a full and fair review.
Internal appeals require the insurer to reassess its decision using all relevant information. For non-urgent claims, insurers must issue decisions within 30 days for pre-service appeals and 60 days for post-service appeals. Urgent care appeals must be resolved within 72 hours.
If the internal appeal is denied, you may request an external review conducted by an independent third party that is not affiliated with the insurer. The external reviewer’s decision is binding on the insurer. Only a small percentage of denied claims are appealed, though available data shows a meaningful share of appealed claims are ultimately overturned.
Appeals require persistence and documentation. You must submit the appeal within required deadlines, typically 180 days from the denial notice, and provide supporting records, including medical documentation, physician statements, or corrected billing information. Many successful appeals result from demonstrating medical necessity or fixing administrative or coding errors.
Best Practices for Claim Success
To maximize your chances of claim approval, follow these well-established strategies:
- Understand your coverage before seeking service: Review your policy’s covered services, exclusions, and prior authorization requirements. Do not assume coverage, verify it in advance.
- Obtain prior authorization when required: Completing the prior authorization process reduces the risk of denial based on lack of pre-approval, even if you disagree with the requirement.
- Use in-network providers whenever possible: Out-of-network claims generally face higher denial rates and increased cost-sharing, depending on your plan type and benefits.
- Keep detailed records: Save all communications with your insurer, including dates, representative names, and reference numbers. Support claims with documentation from your providers demonstrating medical necessity.
- File promptly: Most policies impose strict deadlines for reporting losses and submitting claims. Claims submitted outside these timeframes are often denied, regardless of merit.
- Work with your provider’s billing office: Billing departments regularly manage claims and can help correct coding errors or supply additional documentation needed for approval.
The Broader System Issues
The claims approval process reflects systemic tensions within insurance. Insurers must balance cost control, fraud prevention, and financial sustainability. Policyholders expect coverage for medically necessary or contractually covered services and fair treatment of legitimate claims. Providers seek to deliver appropriate care without excessive administrative barriers.
Recent transparency and regulatory changes aim to address concerns about improper denials. The Centers for Medicare & Medicaid Services (CMS) finalized rules in 2024 requiring Medicare Advantage, Medicaid managed care, and ACA marketplace plans to implement standardized electronic processes for prior authorization and related claims workflows, with compliance beginning in 2026. These rules require faster decisions and clearer, more specific denial explanations.
States are also pursuing reforms, generally focusing on greater transparency, detailed denial notices, and oversight of automated or algorithm-assisted review tools rather than unrestricted use of technology.
Understanding how the claims process works, administrative rules, clinical judgment, and policy interpretation, does not eliminate frustration, but it helps policyholders navigate denials more effectively.
Insurance claims are not automatic, but they are not arbitrary. Every denial must be supported by a documented reason tied to policy language, medical necessity criteria, or procedural requirements, and policyholders have formal appeal rights to challenge decisions they believe are incorrect.